Spinal Manipulation
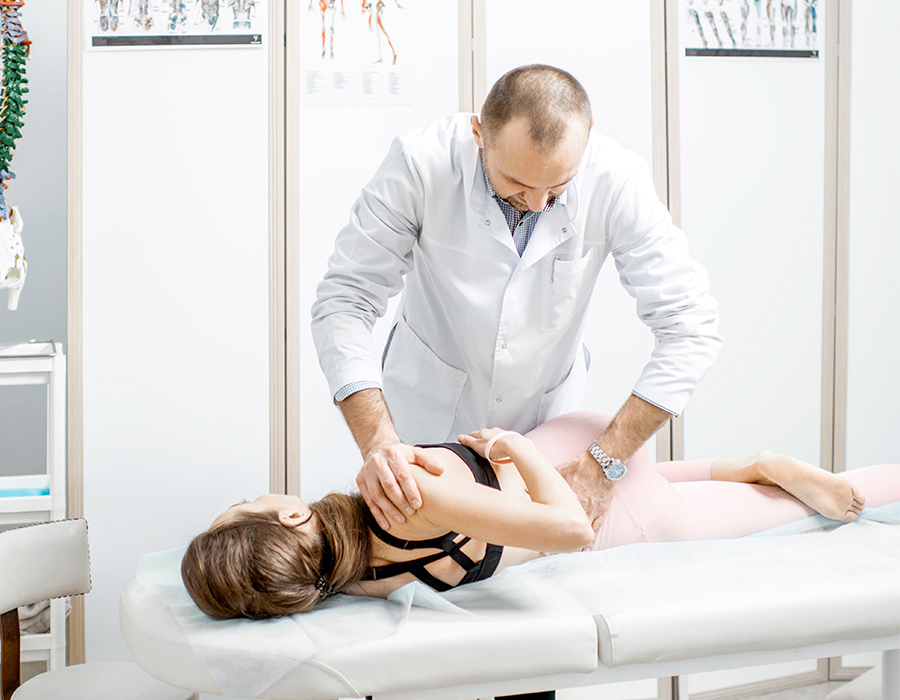
Spinal Manipulation
Spinal manipulation applies a precise, quick thrust to a specific spinal or peripheral joint, taking it briefly beyond its passive range into the paraphysiological space to restore normal joint mechanics and reduce pain. The characteristic ‘pop’ is simply dissolved gas bubbles in the joint fluid — not bones cracking. Manipulation is performed only after thorough assessment and contraindication screening.

CONDITIONS TREATED
- Acute wry neck
- Facet joint syndrome
- Thoracic stiffness
- Sacroiliac dysfunction
- Lumbar hypomobility
- Rib restrictions
- Cervicogenic headache
TECHNIQUES & PROCESS
1. Comprehensive Assessment
Full clinical screen including red flag ruling, neurological testing, and joint mobility assessment to confirm suitability.
2. Pre-manipulation Positioning
Patient positioned to place the target segment at end-range, isolating the specific joint to be treated.
3. HVLA Thrust
A rapid, controlled impulse delivered precisely to the restricted segment, typically producing an audible cavitation sound.
4. Re-assessment and Integration
Immediate post-manipulation reassessment, followed by exercises to reinforce gains in joint range.
KEY BENEFITS
FREQUENTLY ASKED QUESTIONS
Is the cracking sound harmful?
Not at all. The popping or cracking sound — known as cavitation — is simply the rapid formation and collapse of gas bubbles within the synovial fluid of the joint. It is entirely harmless and has no association with joint damage or arthritis. Notably, manipulation can be highly effective even when no sound occurs.
Is spinal manipulation safe?
When performed by a qualified physiotherapist following thorough clinical assessment, spinal manipulation has an excellent safety record. Serious adverse events are extremely rare. The most common side effect is temporary post-treatment soreness that typically resolves within 24 hours. A comprehensive screening is always performed before proceeding.
What is the difference between manipulation and mobilisation?
Mobilisation involves slow, rhythmic, repetitive movements of a joint through its range — the patient remains relaxed and in control. Manipulation is a single, very fast, precise thrust at the end of a joint’s range — it takes milliseconds. Both are effective manual therapy techniques and many physiotherapists use both within the same treatment session.
Who should not receive spinal manipulation?
Absolute contraindications include fractures, bone tumours or metastatic disease, severe osteoporosis, active rheumatoid arthritis at the segment to be treated, progressive neurological deficit, cord compression, and vascular abnormalities. Your physiotherapist will conduct a detailed assessment before every manipulation.
How many sessions will I need?
Many patients feel dramatic improvement after just one or two sessions for conditions such as acute wry neck or facet joint lock. For more complex or recurring problems, 4–6 sessions are recommended — always combined with exercise therapy and postural correction to address the underlying cause and
prevent recurrence.
